Making Molecules Easy to Deliver
In part 1 – we discussed the advantages of transdermal drug delivery and how it offers efficient and economical advantages for patients. We also discussed the skin and what an ideal molecule looks like for drug delivery. Today - we take it one step further.
Cremes, salves and ointments have been used to treat the skin and bodies for centuries. The first adhesive transdermal drug delivery patch approved by the FDA (1979) was for the delivery of scopolamine – to treat motion sickness. Nitroglycerin patches were approved in 1981. Transdermal delivery became widely recognized in 1991, when a nicotine patch for smoking cessation was developed.1
Nicotine, is a very favorable molecule for transdermal delivery. It has a small molecular weight (162.2 Da), adequate lipophilicity (log P = 1.17), low melting point (-67 oC) and is easily absorbed in an alkaline environment (pH ~8.0). Nicotine – through tobacco - can be smoked, sniffed, chewed, or delivered through the outer skin fairly easily2.
When trying to penetrate the skin, most other molecules are not so lucky. When applying an active molecule to the outer skin, you want that molecule to either stay local (topical) or to penetrate deep and be absorbed in the bloodstream (transdermal).

The most common way of topical delivery is to prepare an emulsion. This type of preparation can be a cream, ointment, paste, lotion or gel3. This type of oil/water mixture helps loosen the stratum corneum which allows for penetration of that active molecule tough outer layer and into the lower layers of the epidermis4.
Topical preparations are very easy administer – but require frequent application and it is often difficult to measure the amount of total drug that is applied.
When the desire is transdermal delivery, where the drug penetrates deeper into the skin for systemic absorption, more help is needed. Most of the drugs available in the market today are poorly soluble in water (log P >3) and lipophilic in nature. One area that scientists are shifting their interest is toward nanotechnology lipid based systems – such as nanoemulsification (NE). NE is a leading trend in transdermal drug delivery systems since it enhances drug skin permeation and improves the bioavailability of poorly soluble drugs when compared to other transdermal dosage forms5.

Nanoemulsions (NEs) are colloidal dispersion's of two immiscible liquids, oil and water, in which one is dispersed in the other with the aid of a surfactant / co-surfactant mixture, either forming oil-in-water (o/w) or water-in-oil (w/o) nano-droplets systems, with droplets 20–200 nm in size. NEs are easy to prepare and upscale, and they show high variability in their components6.
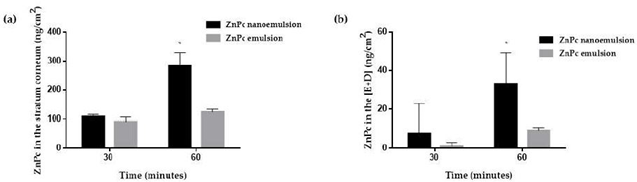
To verify the influence of particle size on skin permeation, an emulsion and nanoemulsion of the highly lipophilic zinc phthalocyanine (ZnPc ; 514 Da, log P = 6,4) was developed and tested on a skin sample. With particles of about 200 nm, the nanoemulsion solubilized 2.5x more than the 13-micrometer emulsion particles.
After 30 minutes of passive delivery, skin treatment with the emulsion or nanoemulsion resulted in similar amounts of ZnPc in the skin. After 60 minutes however, treatment with the nanoemulsion showed 2.3x and 3.6x more ZnPc in the stratum corneum and the epidermis + dermis, than treatment with the emulsion7. This study demonstrates how topical and transdermal penetration can be increased with manipulation of the target molecule.
Whether creating emulsions for topical delivery or more advanced nano-emulsions for transdermal applications, the science of making molecules more deliverable through the skin continues to evolve. Finding ways to make topical and transdermal delivery more efficient could yield better clinical results in a safer, more cost effective and efficient method of drug transport.
In our next piece - we go that second step. We will discuss how different types of patch delivery can take the idea of nanoemulsification even further.
- Margetts, L., Sawyer, R, 2007, https://doi.org/10.10.93/bjaceaccp/mkm033
- Benowitz N.L., Hukkanen J., Jacob P., 2009 https://doi.org/10.1007/978-3-540-69248-5_2
- Common Types of Topical Formulation, http://www.dermweb.com/therapy/common.htm
- Benson, H. Transdermal Drug Delivery: Penetration Enhancement Techniques. Curr. Drug Deliv. 2005, 2, 23–33
- Shrestha, H.; Bala, R.; Arora, S. Lipid-Based Drug Delivery Systems. J. Pharm. 2014, 2014, 801820.
- Skaker, D, et, al., Sci. Pharm.2019, 87(3), 17; https://doi.org/10.3390/scipharm87030017
- Dalmolin, L., Lopez, R., Pharmaceutics 2018, 10, 214; doi:10.3390/pharmaceutics10040214
